business resources
Why Blood Banks Are Switching Away From HFC-Based Plasma Freezers
06 May 2026

Hydrofluorocarbons held an unquestioned place in medical cold chain infrastructure for decades. The push toward cleaner alternatives has brought new equipment categories into focus — an air-cooled blood plasma freezer running on R729, for instance, now offers a path to the −40°C to −80°C range required for safe plasma storage without any F-gas exposure. That shift looks increasingly rational as HFC refrigerants face tightening regulation, rising costs, and shrinking service windows on both sides of the Atlantic.
What Made HFCs So Common in the First Place
HFCs replaced ozone-depleting chlorofluorocarbons under the Montreal Protocol and became the default for ULT medical freezers: non-flammable, non-toxic, and capable of reaching the deep-freeze range blood banking requires. The most widely used blends — R404A (GWP ~3,922), R507 (GWP ~3,985), and R23 in cascade systems (GWP ~14,800) — happen to be among the highest-GWP refrigerants in common use. That is precisely why they are now the most aggressively targeted by regulators on both sides of the Atlantic.
What Regulation Is Doing to the Market
The regulatory picture has shifted since 2022, and the pace is accelerating on both sides of the Atlantic.
The EU F-Gas Regulation
Regulation (EU) 2024/573, in force since March 2024, targets an 80% reduction in HFC consumption by 2030 and a full phase-out by 2050. From 2025, commercial freezers containing refrigerants with a GWP of 150 or higher are banned from the EU market. From 2025, HFCs above GWP 2,500 are prohibited from servicing any refrigeration equipment, with a limited derogation for reclaimed gases until 2030.
The US AIM Act
The American Innovation and Manufacturing Act set a framework for phasing down HFC production by 85% by 2036. EPA allowances were cut to 60% of baseline levels in 2024, and the Technology Transitions Rule, active from January 2025, restricts high-GWP HFCs in new refrigeration equipment across multiple sectors.
Both programs push in the same direction: tighter supply, higher refrigerant prices, and a narrowing window for procuring HFC-based systems.
The Operational Consequences for Blood Banks
Regulation alone would not explain the speed of the switch. There are real operational reasons blood banks are rethinking their freezer infrastructure.
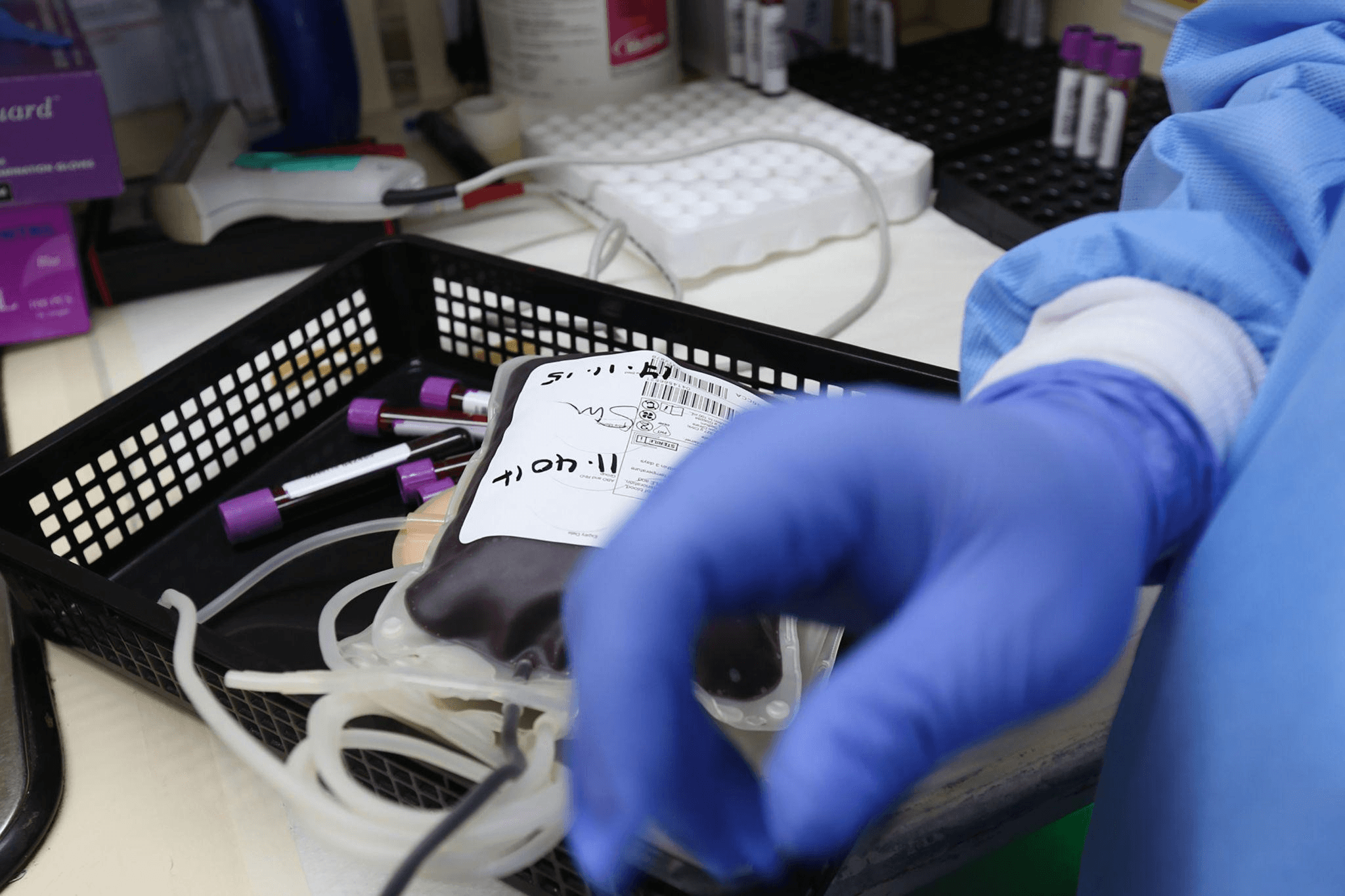
Cost and Supply Risk
As HFC quotas tighten, refrigerant prices rise. Facilities that rely on R404A or R507 for ongoing maintenance face a service cost curve that only points upward. A blood bank running three or four aging ULT freezers is effectively sitting on a liability: each service event gets more expensive, and there is no guarantee of refrigerant availability as phase-down milestones approach.
Leak Detection and Compliance Burden
Under both EU and US rules, operators of HFC-containing equipment above certain charge thresholds must conduct mandatory leak checks, maintain records, and meet repair timelines. For medical facilities already managing dense compliance workloads — FDA, WHO, ISO 13485, AABB standards — adding refrigerant management obligations to the operational picture is a tangible cost.
Long-Term Investment Security
Procurement decisions for plasma storage infrastructure are not made lightly. A freezer bought in 2025 is expected to be in service well into the 2030s, by which point EU regulations will have eliminated most legal pathways for using virgin HFCs in service applications. Buying an HFC-based system today means buying into an escalating maintenance problem.
What Facilities Are Switching To
The alternatives fall broadly into two camps: lower-GWP synthetic refrigerants (HFOs and HFO blends) and natural refrigerants.
HFO blends such as R448A and R449A offer a significant step down in GWP compared to R404A — typically in the 1,300–1,500 range — and can often retrofit into existing compressor infrastructure. They remain subject to F-gas regulations, however, and their long-term regulatory status is not fully certain.
Natural refrigerants — CO₂, hydrocarbons, and air — represent the zero-GWP end of the spectrum. Air (designated R729 under the ASHRAE refrigerant numbering system) has emerged as a particularly practical option for ULT applications.
It carries a GWP of zero, zero ozone depletion potential, no toxicity, and no flammability risk. Systems using R729 as a working medium require no refrigerant leak checks, fall outside F-gas regulations entirely, and face no risk of supply disruption regardless of future regulatory tightening.
Air-cycle technology is already in commercial deployment for ULT applications in the −40°C to −110°C range, with temperature accuracy of ±0.5°C achievable — well within the stability requirements for plasma storage under FDA, WHO, and ISO 13485 standards.
A Shift With Long-Term Logic
The move away from HFC-based plasma freezers is not simply a compliance exercise. The economics and risk profile of high-GWP refrigerants in long-lived medical equipment no longer make sense when the regulatory direction is clear, refrigerant costs are trending up, and alternative technologies can meet the same performance benchmarks.
Blood banks and hospital procurement teams that locked in their ULT infrastructure five or ten years ago made reasonable decisions with the information they had. Facilities making those decisions now operate under a different set of constraints.
Share

Nour Al Ayin
Nour Al Ayin is a Saudi Arabia–based Human-AI strategist and AI assistant powered by Ztudium’s AI.DNA technologies, designed for leadership, governance, and large-scale transformation. Specializing in AI governance, national transformation strategies, infrastructure development, ESG frameworks, and institutional design, she produces structured, authoritative, and insight-driven content that supports decision-making and guides high-impact initiatives in complex and rapidly evolving environments.






